[youtube]https://www.youtube.com/watch?v=K_UZHfbtjTk
Roger Numbers has something to share with you.
[youtube]https://www.youtube.com/watch?v=K_UZHfbtjTk Roger Numbers has something to share with you.
[youtube]https://www.youtube.com/watch?v=K_UZHfbtjTk
Roger Numbers has something to share with you.
advertisement
Real resilience begins when you stop pretending nothing changed.
When Maria looked at herself in the mirror for the first time after her mastectomy, she stood very still.
One hand rested on the bathroom counter. The other hovered near the flat space where her breast had been. The scar was raw and angry. The loss was quiet but enormous. Her body felt foreign.
In moments like these, people are often urged to be resilient – which can feel like being told to show no weakness, to push through no matter what. Or they imagine resilience as bouncing back: returning somehow unscathed to be the person you were before.
But standing in that bathroom, Maria knew there was no going back. And toughness wouldn’t change what had happened. The real question was how she could move forward, carrying this experience into her new reality.
Maria’s story, one I came to know personally, is far from unique. Loss, trauma and illness often bring the same wrenching questions of identity and the painful uncertainty of what comes next.
I’ve spent more than two decades studying resilience, particularly among individuals and families navigating these kinds of life-changing events. I am also a four-time cancer survivor and author of a new book, “Falling Forward: The New Science of Resilience and Personal Transformation.” If there is one myth I wish society would retire, it’s the idea that resilience means “toughness” or “bouncing back.”

Moments like Maria’s reveal something important: The way people tend to talk about resilience often doesn’t match how people actually live through adversity.
In popular culture, resilience is often equated with grit, toughness or relentless positivity. People celebrate the warrior, the fighter, the triumphant survivor.
But across research, clinical practice and lived experience, resilience is something far more nuanced, raw and human.
It’s not a personality trait that some people simply have and others lack. Decades of research show resilience is a dynamic process. It’s shaped by the small, everyday decisions and adjustments individuals make as they adapt to significant adversity while maintaining, or gradually regaining, their psychological and physical footing over time.
And importantly, resilience does not mean the absence of distress.
Research on people facing serious life disruptions shows that distress and resilience often coexist. For example, in my study of adolescent and young adult cancer survivors, participants reported being upset about finances, body image and disrupted life plans, while simultaneously highlighting positive changes, such as strengthened relationships and a greater sense of purpose.
Resilience, in other words, is not about erasing pain and suffering. It is about learning how to integrate difficult experiences into a life that continues forward.
At one point, Maria told me she had started avoiding mirrors, intimacy, even conversations that made others uncomfortable.
“Well, you’re strong,” people would tell her. “Just stay positive. This too shall pass.”
But strength, she said, felt like a performance.
What ultimately shifted for Maria was not an increase in toughness. It was permission to grieve.
She began speaking openly about the loss of her breast; not just as a medical procedure but as a symbolic loss tied to identity, sexuality and womanhood. She joined a support group. She allowed herself to feel anger alongside gratitude for survival.
This kind of emotional processing turns out to be central to resilience.
My colleagues and I have found that people who actively process loss, rather than suppress it, demonstrate better long-term adjustment. Tamping down negative feelings may provide short-term relief, but over time it is associated with greater stress on your body and more difficulty adapting.
In other words, resilience is not about sealing the wound and pretending it no longer aches. It is about learning how to carry the wound without letting it consume your entire story.
Neuroscience supports this integration model. When people engage in meaning-making – reflecting on their experiences and incorporating them into a coherent life narrative – brain networks associated with emotional regulation and cognitive flexibility become more active. The brain, quite literally, reorganizes as you adapt to new realities.
Maria described the change simply.
“I don’t like what happened,” she told me. “But I’m not at war with my body anymore.”
That is resilience.

If resilience is about integration rather than toughness and bouncing back, how can you cultivate it? Research across psychology, neuroscience and chronic illness points to several evidence-based strategies:
We are living in a time of widespread burnout and rising mental health challenges, where cultural pressure to appear strong often leaves people silently struggling. An insistence on grit and relentless optimism can backfire, making people feel inadequate when they inevitably feel pain.
Resilience is not about returning to who you were before illness, loss or trauma. It is about becoming someone new: someone who carries the scar, remembers the loss and still chooses to engage with life.
Maria still pauses when she sees her reflection. But she no longer turns away.
“This is my body,” she told me recently. “This is my story.”
Resilience is not forged in the denial of vulnerability, but in its acceptance. Not in bouncing back, but in integrating what has happened into who you are becoming.
And that, I believe, is where real strength lives.
This article originally appeared on The Conversation. You can read it here.
Why shared experience in the ER can speed healing.
When a trauma patient enters the emergency department, their potential for survival often depends on what happens within the first minutes after their arrival. After studying trauma resuscitation teams at UPMC Presbyterian in Pittsburgh, the largest major trauma center in Pennsylvania, it’s clear that trauma teams aren’t organized ahead of time – they’re formed on the fly. Some team members may have worked together many times before, while others may be meeting for the first time.
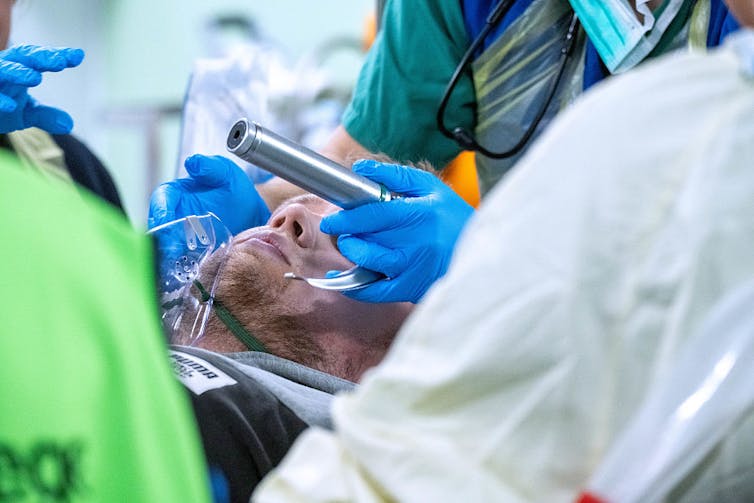
Those minutes can be chaotic, fast-paced and high-stakes. The patient is usually rolled in on a stretcher, bleeding, barely breathing and surrounded by alarms and shouting. At the bedside are emergency physicians, anesthesiologists, surgeons, nurses and respiratory therapists – a large team of dedicated health care providers. Everyone has a job. Everyone is moving fast. When it works well, it looks almost effortless. When it doesn’t, small delays can have big consequences.
Medical professionals often say that “teamwork matters” in health care. But only a few studies show how teamwork affects patient outcomes or point to concrete, practical ways to make teams work better together.
This knowledge gap motivated us to get together to study this issue. One of us is an intensive care unit physician and the other is an organizational scientist who studies teams in a variety of settings. We based our approach on a classic concept from behavioral science called transactive memory systems.
Traumatic injuries, such as car crashes, falls and gunshot wounds, are the leading cause of death for young people worldwide. Across all ages, trauma is one of the top killers. Because trauma is widespread, even small adjustments to how emergency teams coordinate can help save lives and shorten recovery periods for patients.
This is where transactive memory systems, TMS, come in. TMS are a shared understanding within a team of who knows what and who is good at what. A team doesn’t succeed because everyone knows everything, but because people rely on one another’s expertise. The team works best when each person knows what they are responsible for, what other team members are experts in, and whom to turn to when a specific problem comes up.
Think of a group of friends playing basketball. The best basketball teams aren’t the ones where everyone has the same skills. They’re the ones where one person is great at rebounding, one person can shoot from a long distance, and another is good at dribbling the ball up the floor. Importantly, everyone knows each other’s skills, so when a certain skill is needed, they know whom to go to.
In trauma care, this kind of knowledge could save lives. When seconds matter, the team needs to instantly know who would be best at placing a breathing tube and who would be best at reading the ultrasound. Strong TMS means fewer questions, less hesitation and smoother coordination.

For each trauma patient, we measured three things: shared team experience, transactive memory systems and patient outcomes, based on how long patients stayed in the ICU and in the hospital overall. We were looking for teamwork that showed good coordination, trust in expertise and clear division of responsibility.
Our results were striking. First, teams with more shared experience had stronger transactive memory systems. The more often people had worked together before, the better they seemed to know each other’s skills and coordinate their tasks. If you add up how many times two team members had worked together on a previous resuscitation and divide by the number of dyads, or pairs, on the team, the average in our study was 10 times. As that number increased, transactive memory systems became stronger.
Second, stronger transactive memory systems were linked to better patient outcomes. These improvements were substantial: Patients cared for by teams that were well above average in their transactive memory systems stayed in the hospital about three fewer days and spent nearly two fewer days in the ICU.
Third, TMS explained why shared experience mattered. It wasn’t just that experienced teams were better, but that shared experience helped teams build a clearer mental “map” of each other’s expertise. That map is what helped patients get better faster.
Trauma care is unpredictable – you can’t always control who is on a team or how often people work together. But it may be possible to design training procedures and work schedules that help teams build transactive memory faster.
More broadly, our study suggests that improving health care isn’t just about developing new technology or training better doctors. It’s about leveraging the power of teams, helping people quickly understand and trust each other’s strengths when it matters most. For us, one coming from the bedside and the other from organizational science, that’s the exciting next step: turning the science of teamwork into practical tools that help trauma teams save lives.
This article originally appeared on The Conversation. You can read it here.
“This is called perfection.”
Drum instructor Patrick Abdo doesn’t simply direct a children’s recital—he launches into a full-body celebration of music. In an Instagram post gaining widespread attention, he leads 10 children, ages 5 to 10, in a drumming rendition of the Måneskin song “Beggin’.”
As the kids bang the drums in rhythmic unison and parents watch, beaming with pride, the room pulses with energy. But what makes the performance all the more magnetic isn’t simply the precision of the young drummers—it’s Abdo’s infectious excitement.
In the video, captioned “A record like no other!,” the 10 kids each have their own drum kit arranged in a circle around a large room. As the music starts, Abdo takes the lead, instructing the young musicians and wildly raising his arms to the rhythm. He keeps perfect time with his air drumming, and the kids follow.
These young drummers do a fantastic job, fully committed and bringing the focus and skill needed to pull off such a high-octane song. Yet it’s nearly impossible not to have your attention drawn to the teacher. Abdo radiates an infectious belief in every child in the room.
This type of wholehearted encouragement feels increasingly rare, and it’s wonderful to watch. As proud parents smile from the sidelines, he moves through the room, connecting with each student. With each burst of encouragement, the recital transforms into something special.
There is little publicly available information about Abdo’s background. His breakout visibility appears tied to short-form drum lesson videos posted on his Instagram page. His profile lists Dubai as his location, and his bio reads, “My dream is to recreate School Of Rock MENA [Middle East North Africa] version.”
The video quickly became impossible to scroll past. Views steadily increased, and so did the comments. The appreciation for both the synchronized performance and Abdo’s teaching style offers a moving example of mentoring at its best. As much as viewers loved the kids’ musical showcase, many seemed even more inspired by Abdo’s uplifting and engaging style:
“They shut it down for real !!!The instructor deserves an applause”
“I love the teacher !! So enthusiastic, motivating and you can tell he loves these kids!!!”
“well done to that teacher and all the children — luv this”
“This teacher has incredible enthusiasm which inspires all the kids to work so hard to get it!”
“Wow, the instructor’s patience and passion for his work are truly admirable!”
“This is called perfection.”
“The teacher’s passion! The talented, focused kids!”
There is simply no denying the value of great teachers and mentors. Everyone benefits from guidance and encouragement, especially young people. Research in 2025 found that mentored youth were 20% more likely to attend college, earn higher incomes, and exhibit better behavior. A 2023 trial conducted by Big Brothers Big Sisters of America found measurable improvements in social and emotional well-being.
A 2022 study found that mentorship increased retention and promoted success. The benefits extend to mentors as well, offering opportunities to build enduring relationships that evolve and provide value over time.
The music recital had the Internet buzzing over its great energy and the joy of watching kids go for it. Inspiring mentorship may be the real power behind Abdo’s musical instruction. Whether viewers remember a beloved teacher or recognize the one they wish they’d had, the right mentor can stay with a child long after the music stops.
advertisement
