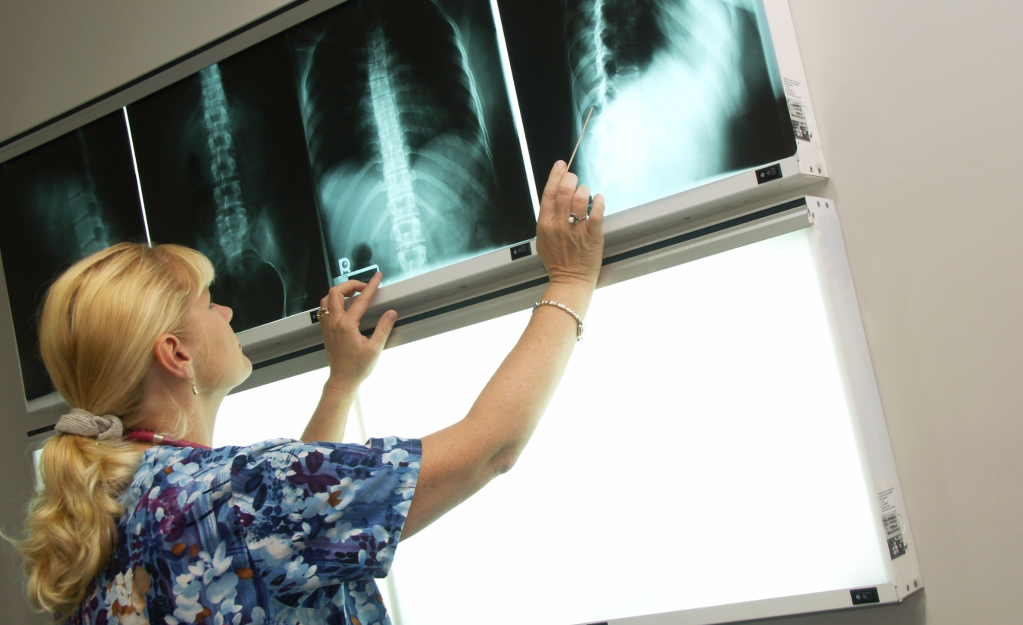
It’s important for the world to understand the seriousness of COVID-19. It’s not “just like the flu.” It’s not like a “bad cold.” It’s a serious virus that kills, especially elderly people.
Michael Bane, a 42-year-old Vice President of Client Engagement at Deighan Law, LLC, wanted the world to know just how serious the coronavirus is so he posted a brutally honest, harrowing account of his first eight days with the disease on Facebook.
Bane is a healthy man who two weeks ago did “13 pullups and ran a sub-seven mile” and has ran six miles with a torn tendon. So, he assumed that the coronavirus isn’t a serious concern. ” I am in shape,” he says in his Facebook post. “I am a tough guy.”
But over the course of eight days Bane learns that COVID-19 is a serious, life-threatening condition that everyone, regardless of their age, should take seriously.
The account published below goes through March 20. As of this article’s publication, Bane is still in the hospital’s ICU unit and is hopeful he will recover.
Here’s his original Facebook post, below is an abridged version.
For all those who have asked the question “Does anyone even know anybody that has gotten the coronavirus?”, if you know me, you do now. My positive test for COVID-19 has been relayed to me, and I wanted to share what my experience with this illness has been.
Thursday, March 12.
I’m at home eating spicy Chinese food (ignore any apparent irony) and my nose starts running, very mildly. I’m assuming it’s from the hot and sour soup. I don’t have to wipe it, blow it, or anything. It goes away within an hour and wasn’t something that would have registered if not for the current COVID-19 pandemic.
Friday, March 13
Nose is slightly runny in the morning. Clears up shortly, nothing else. I have no need to wipe my nose or use a tissue.
Saturday, March 14
Slight sore throat. No sniffles at the moment, but I assume it’s from post-nasal drip or possibly due to sleeping without the humidifier, which is normally on at night.
Sunday, March 15
My cough is more persistent. The sore throat is worse, but it goes away quickly again. My nose has stopped running. My Google searches tell me it could be COVID-19, but it could be any number of other things. I am slightly worried and try to trace back to where I could have been exposed.
I can’t sleep. For whatever reason I just cannot get comfortable. I keep tossing and turning trying to alleviate this backpain on my left side, but nothing is working. At 1 am, it occurs to me this might not be normal backpain. I’m sleeping in the guest room at this point, because I don’t want to keep my wife up. I take my temperature. It’s 100.5, a slight fever.
Bane decides to schedule a virtual appointment with a doctor.
Monday, March 16
Scheduling a video appointment is difficult, as I keep getting the “we’re at capacity, please try again later” message. I finally manage to secure one ($49, pre-paid), and find myself face to virtual face with a physician’s assistant about two hours later. She reviews my symptoms and circumstances (worsening cough, annoying fever, bad pain), and due to potential for exposure, says I should get tested. She puts a request in with the hospital and says it will be 1-5 days. I should head to the ER if I start having trouble breathing.
My fever is 102.5. My left hand is tingling, my oxygen saturation is down. I tell myself this is because of an increased respiratory rate due to the fever, not because corona has attacked my lung function. I’m right, but the thought still worries me. My wife tells me to take Tylenol or Advil. I tell her no; I’m going to kill the virus off with heat. I tell the virus to buckle down, because it’s about to burn in Hell.
My wife hears me laughing at something. I don’t know what. She asks me to take my temperature. I adjust myself on the bed and an arctic blast hits my body. My skin is on fire. This doesn’t feel right at all. I run various death scenarios through my mind to see if this situation fits. I feel that bad. I check the thermometer, and my wife again presses me for the temperature.
I wake up at around 1:30 am with a sudden desire to use the facilities. As I’m sitting on the commode, I smell something bad. I realize I’m also soaking wet. The smell is me. I have sweat so much my shirt is drenched like I’ve just done the polar bear plunge. It’s disgusting. I strip out of my pajamas and find another pair.
Tuesday, March 17
I need this test. The fever is back, 100.8, and the cough is worse. I feel better than yesterday, but I am dreading what’s to come. I shower and get my daughter ready for daycare. I don a mask and drop her off.
Bane arrives at the hospital.
A hospital employee steps out in a mask and motions for me to get out of the car. My own mask is on, and I do. He immediately instructs me to put my hands in my pocket and not to remove them. He unlocks a door, and I follow him inside. I am again told not to take my hands out, and it’s added that I shouldn’t touch anything either. This seems redundant, unless he is telling me not to touch the insides of my pockets, in which case, I am not in compliance.
The doctor at the end of the hall is dressed like she’s about to enter Chernobyl.
She explains the nasal swab process and says that the probe is going to go in REAL DEEP. She repeats it for emphasis. I nod, and cough. I weigh whether knowing is worth this nasal intrusion. I lower my mask below my nose and look up. It’s mildly uncomfortable, but not nearly as bad as I was expecting.
Tuesday, March 18
It’s been two weeks since I was exposed. I wake up drenched in sweat again and take a 5 am shower. I go back to sleep for a bit and am rudely woken up by an alert on my phone. My test results are back already. That was fast. I go to the app to find out that I am negative for Influenza A and B.
Around 6 pm I have a horrible coughing fit. Every one of my shallow breaths is met with a corresponding respiratory spasm as the air is forced back out of my lungs. It goes on and on and on. My wife asks me if I need to go the hospital. That seems like an overreaction, but my coughing doesn’t allow me to reply. I wave her off and continue hacking and wheezing. I’m fighting for air, but I believe it’s going to pass
Thursday, March 19
I wake up freezing cold, and in horrible pain. My left lat seizes up, feeling like it’s trying to rip itself in half. As I attempt to figure out how to relax it, my foot cramps painfully as well. I am massively dehydrated. I’m drinking a lot of water, but the lack of food is keeping me from retaining much.
When am I going to turn the corner? When is this all going to end? To everyone who said it was just a bad cold or like the flu, or that people were far more likely to be asymptomatic: fuck you.
Friday, March 20
I get into a few arguments with people on social media regarding the term “Chinese Virus” and the inherent racism behind it. My opinion as an Asian-American is quickly and skillfully invalidated with well-crafted lines of reasoning such as “Just another snowflake” and “KISS MY ASS” (caps not mine). Clearly, the only thing I have proven is that I still haven’t learned what a waste of time arguing on social media is.
Later that day, Bane drove himself to the hospital.
My phone rings. The Illinois Department of Health calls to tell me I’m positive for COVID-19. I laugh and reply that I could have told them that.
I text my family, a few close friends, and my boss. Everyone is very kind. My boss lets me know they’re going to have to inform the office someone tested positive, but they’ll keep my anonymous. I tell him to use my name. It’s a scary message to get, and if people have questions maybe I can help. People may take social distancing protocols more seriously if there’s a face to associate with the illness. By the way work people, expect a message sometime soon.
I get into the ER and they take a chest X-ray. I have bilateral pneumonia. This explains the crackling sounds I’ve been hearing when I breath. My fever is 102. I’m admitted, stuck with an IV, and a host of medications are prescribed to me both intravenously and otherwise
So here I am, in the hospital on the 13th floor with a lovely view of the city. Take that isolation! The coughing won’t stop, and I’m waiting for the drugs to arrive. My prognosis seems reasonably good, I don’t need oxygen yet, and the monitors will keep an eye on my levels.
The point of all this? It’s not real for some of us until it happens to us or someone we know. I appreciate the well-wishes I’ve gotten and am bound to get, and don’t want your sympathy. Please please PLEASE take this seriously. This could kill me. Practice social distancing.
People have died. People will die. It might be people you love. Please stay inside. This is horrible, brutal, devastating and it feels l might be cashing my chips in. Protect the people you care about as best you can. I love you all.