A patient of mine, a veteran who had tried to quit smoking for over a decade, told me that after he started a GLP-1 drug for his diabetes, he lost interest in cigarettes. He didn’t use a patch. He didn’t set a quit date. He simply lost interest. It happened without effort.
Another patient on one of these drugs for weight loss told me that alcohol had lost its pull – after years of failed attempts to quit.
People struggling with many addictions, ranging from opioids to gambling, are reporting similar experiences in clinics, on social media and around dinner tables. None of them started these drugs to quit. This pattern of people losing their cravings across a broad range of addictive substances has no precedent in medicine.
But my patients were giving me an important clue. People taking GLP-1 drugs often talk about “food noise” vanishing: the constant mental chatter about food that dominated their days simply goes quiet. But my patients were reporting that it wasn’t just food: They were noticing that the preoccupation with smoking, drinking and using drugs that drives people back despite their best intentions to stop was going quiet too.
As a physician whose patients are often on GLP-1 drugs, and as a scientist who works on answering pressing public health questions – from long COVID to medication safety – I saw a problem hiding in plain sight: Many addictions have no approved treatment. The few medications that exist are massively underutilized, and none works across all substances. The idea that a drug already taken by millions might do what no addiction treatment has done before was too important to ignore.
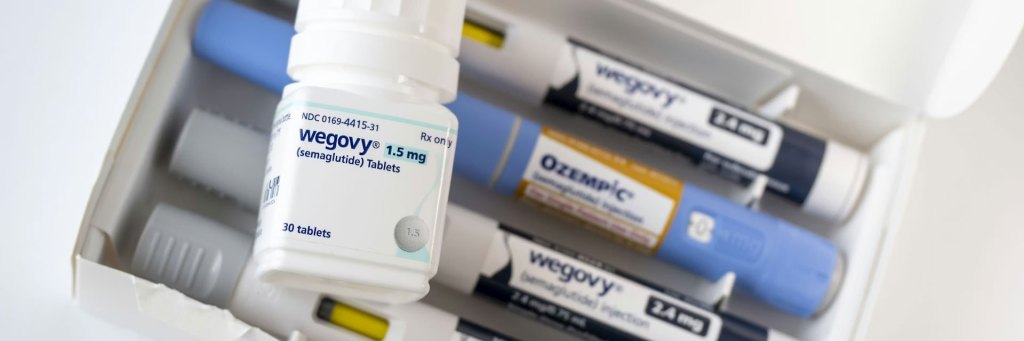
My team and I set out to test whether GLP-1 drugs – medications like semaglutide (Ozempic and Wegovy) and tirzepatide (Mounjaro and Zepbound), originally developed for diabetes and then approved for obesity – could do what no existing addiction treatment does: curb craving itself.
Our evidence strongly suggests they can.
Biological basis of cravings
The hormone that these drugs mimic – GLP-1 – is not only produced in the gut. It is also active in the brain, where the receptors it binds to cluster in regions governing reward, motivation and stress – the same circuitry that gets hijacked by addiction. At therapeutic doses, GLP-1 drugs cross the blood-brain barrier and dampen dopamine signaling in the brain’s core reward center, making addictive substances less rewarding.
GLP-1 drugs seem to inhibit cravings for several different substances in multiple animal models. For instance, rodents given GLP-1 drugs drink less alcohol, self-administer less cocaine and show less interest in nicotine. When researchers gave semaglutide to green vervet monkeys – primates that voluntarily drink alcohol much like humans do – the animals drank less without showing signs of nausea or changes in water intake. This suggests the drug lowered the reward value of alcohol rather than making the animals feel sick.
From animals to people
To find out whether these drugs have a similar effect on people, we turned to the electronic health records of more than 600,000 patients with Type 2 diabetes at the U.S. Department of Veterans Affairs – one of the largest health care databases in the world.
We designed a study that applied the rigor of randomized controlled trials – the gold standard in medicine – to real-world data. We compared people who started GLP-1 drugs to people who did not, adjusting for differences in health history, demographics and other factors, and followed both groups for three years.
My team and I asked two questions: For people already struggling with addiction, did the drugs reduce overdoses, drug-related hospitalizations and deaths? And for people with no prior substance use disorder, did GLP-1 drugs reduce their risk of developing one across all major addictive substances: alcohol, opioids, cocaine, cannabis and nicotine?
What we found was striking. In the group already struggling with addiction, there were 50% fewer deaths due to substance use among those taking GLP-1 drugs compared with those who were not. We also found 39% fewer overdoses, 26% fewer drug-related hospitalizations and 25% fewer suicide attempts. Over three years, this translated to roughly 12 fewer serious events in total per 1,000 people using GLP-1 drugs – including two fewer deaths.
Reductions of this magnitude are rare in addiction medicine – and what’s remarkable is that the finding came from drugs initially designed for diabetes, later repurposed for obesity and never intended to treat addiction.
The drugs also appeared to prevent addiction from developing in the first place. Among people with no prior substance use disorder, those taking GLP-1 drugs had an 18% lower risk of developing alcohol use disorder, a 25% lower risk of opioid use disorder and an approximately 20% lower risk of cocaine and nicotine dependence. Over three years, this translated to roughly six to seven fewer new diagnoses per 1,000 GLP-1 users.
With tens of millions of people already using GLP-1 drugs, the reductions in deaths, overdoses, hospitalizations and new diagnoses could translate into thousands of prevented serious events each year.
Converging evidence
Our findings align with a growing body of evidence.
A Swedish nationwide study of 227,000 people with alcohol use disorder found that those taking GLP-1 drugs had 36% lower risk of alcohol-related hospitalizations. This is more than double the 14% reduction that the same study found with naltrexone, which was the best-performing medication approved for treatment of alcohol use disorder in that analysis. Other observational studies have linked GLP-1 drugs to lower rates of new and recurring alcohol use disorder, reduced diagnoses and relapse in cannabis use disorder, fewer health care visits for nicotine dependence and lower risk of opioid overdose.
Meanwhile, randomized controlled trials that directly test whether these drugs help people with addiction also show promise. In one trial, semaglutide reduced both craving and alcohol consumption in people with alcohol use disorder. In another, dulaglutide reduced drinking. More than a dozen additional trials are already underway or actively enrolling, and several more are planned.
The future of addiction treatment
GLP-1 drugs are the first type of medication to show potential benefit across multiple substance types simultaneously. And unlike existing addiction medications, which are prescribed by specialists and remain vastly underused, GLP-1 drugs are already prescribed at enormous scale by primary care doctors. The delivery system to reach millions of patients already exists.
The consistency of GLP-1 effectiveness across alcohol, opioids, cocaine, nicotine and cannabis suggests these drugs may act on a shared vulnerability underlying addiction – not on any single substance pathway. If confirmed, that would represent a fundamental shift in how society understands addiction and how doctors treat it.
Some unanswered questions remain, though, about how these drugs would affect addiction. Many people who take GLP-1 drugs to treat obesity or diabetes discontinue them; afterward, their appetite typically returns and they regain the weight they lost. Whether the same rebound would occur with addiction, and what it would mean for someone in recovery to face the roar of craving again, is unknown. Nor is it clear whether the benefits persist over years of continuous use, or whether the brain adapts in ways that dampen those effects.
Also, because GLP-1 drugs engage the brain’s reward circuitry – the same system that governs not just craving but everyday motivation – prolonged use could, in theory, dampen motivational drive in some people. Whether that might affect real-world outcomes, such as initiative, competitive drive or performance at work, remains an open question.
What comes next
GLP-1 drugs have not been approved for addiction, and there is not yet enough evidence to prescribe them solely for that purpose. But for millions of people already weighing whether to start a GLP-1 drug for diabetes, obesity or another approved indication, it is one more factor worth considering.
A patient living with diabetes who is also trying to quit smoking might reasonably choose a GLP-1 drug over another glucose-lowering medication, not because it is approved for smoking cessation, but because it may help them quit, a benefit that other diabetes drugs do not offer. Similarly, for people living with obesity who also struggle with alcohol, the potential for benefit beyond weight loss could be one more reason to consider a GLP-1 drug.
If additional trials confirm that they effectively curb cravings across addictive substances, these drugs could begin to close one of the most consequential treatment gaps in medicine. And the most promising lead in addiction in decades will have come not from a deliberate search but from patients reporting a benefit no one anticipated. Like my patient who quit smoking after a lifetime of trying, it happened without effort.
This article originally appeared on The Conversation. You can read it here.